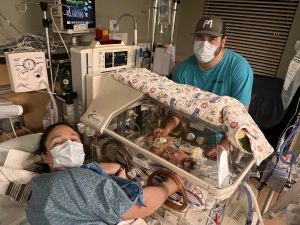
 Preemie: Blake Rakotz
Preemie: Blake Rakotz
Gestation at Birth: 33 weeks
Days in the NICU: 17 days
Parent: Jennifer Poelstra
“God made me so that you can see small things are strong too.”
Preemie Story:
At 19 weeks, I had my anatomy scan, which revealed I had placenta previa. At 27 weeks, I woke up to vaginal bleeding. My husband immediately took me down to the main hospital (not one of the satellites that are closer, just in case Blake would need to come early). On the way down, I never felt a kick (which was hard to feel regardless due to being in a moving car and he was still very small). We thought we lost him. Upon arrival, they checked his heart rate/ did another anatomy scan and he was perfectly fine (thank goodness). It was the placenta that was bleeding. I was admitted for a day and discharged.
I had a follow up with my OBGYN the following day, who wanted me removed from work due to working a physically demanding job. I negotiated with my OB and husband to return to work on light duty and do nothing at home. They agreed. I returned to work for exactly 2 weeks and at 29 weeks, I experienced my second bleed. Again, thankfully, Blake was fine and healthy. This bleed was extremely emotionally hard on me, as I had to walk away from work and go on leave. Don’t get me wrong, I love my son very much and wanted what was best for him. But my career was my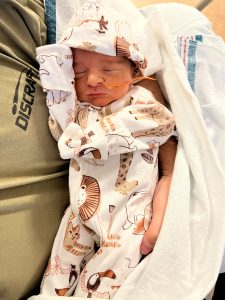 identity up until this pregnancy. It is what I went to school for, for 8 years. After two days, I was discharged. Discharged knowing 1: I was done with work and 2: If I was to have a third bleed, I would be admitted to the hospital until birth.
identity up until this pregnancy. It is what I went to school for, for 8 years. After two days, I was discharged. Discharged knowing 1: I was done with work and 2: If I was to have a third bleed, I would be admitted to the hospital until birth.
Luckily I was able to have my baby shower as planned, but unfortunately, I experienced my third bleed at 31 weeks. Before leaving the house, I delayed a little bit (I felt Blake kicking so I was reassured by his movements). I packed a large suitcase, spent a little extra time with my dogs and then headed out. The goal was to make it to 36 weeks.
I knew this hospitalization had the potential to be 5 weeks long. Upon admission, more imaging was done and thankfully, Blake was healthy. I was given a rescue dose of betamethasone in preparation for a possible delivery. Over the next few weeks I remained in the hospital with multiple bleeds. The 5th bleed I was given the second dose of betamethasone and as they put my baby on the monitors, they couldn’t find a heartbeat. After an emergency was called and I had about 3 OB doctors in my room, they found his heart beat. I met with the NICU team, MFM doctors and of course my OB team. The goal was always 36 weeks but MFM decided after 34 weeks, if I was to have any bleeding at all, they would do an emergency C section.
After 15 days in the hospital (including Christmas) and 3 bleeds, they decided to do an emergency C section due to the heaviness of the sixth bleed. I had my mom and sister present when the 6th bleed happened and the decision was made for an emergency c section. The OB team was kind enough to give my husband time to get to the hospital before they called a category 2 emergency c section.
On 12/29/22, at 33 weeks, Blake was delivered and immediately taken away. I wasn’t able to see him for 4 hours after delivery but my husband was able to bounce between me in the OR, recovery, and mother baby unit and the NICU. Blake was 5lbs, 7ozs and 18 inches long. He was diagnosed with respiratory distress syndrome and was breathing with assistance from a C-pap with the vent. He also was in the incubator to help him maintain temp. At 1 day old his breathing worsened and he was intubated and given surfactant into his airway. After this procedure, his breathing significantly improved. The next few days he was weaned off supplemental oxygen, was taking food all by mouth, and was able to keep the top off of his incubator. One evening after we left, he declined significantly in all areas (breathing, oral intake, and maintaining temperature). He was placed back on a C-pap with a vent, had a og tube placed for food, and was back in his incubator. The neonatologist ran multiple labs and some twice checking for sepsis due to the quick decline. All labs came back within normal limits and they honestly think they pushed too hard too fast and as they stated “he was reminding us he is only 33 weeks gestation”.
 After this episode, we slowly weaned him off oxygen, then once on room air and saturating appropriately, worked on feeding, and once feeding was all orally (but still had NG tube in), we worked on the temperature regulation. We decided to break apart the three areas vs. work on them all at once due to the major setback we had experienced and this gave him time to process each change.
After this episode, we slowly weaned him off oxygen, then once on room air and saturating appropriately, worked on feeding, and once feeding was all orally (but still had NG tube in), we worked on the temperature regulation. We decided to break apart the three areas vs. work on them all at once due to the major setback we had experienced and this gave him time to process each change.
Blake was in the NICU for a total of 17 days. Those 17 days we felt every emotion, from guilt, sadness, scared, thankfulness, and happiness. The things that made those 17 days easier was:
1. Excellent communication with the NICU team
2. Seeing the NICU nurses with the patients (not just Blake but all the other babies).They showed so much empathy and compassion and provided love and comfort to their patients by holding them, talking to them, or just touching them when they were in the incubator to let them know they are okay.
and compassion and provided love and comfort to their patients by holding them, talking to them, or just touching them when they were in the incubator to let them know they are okay.
3. Family support. We had family and friends reach out/ check in on us, provide help with caring for our dogs as we spent long days at the hospital to be with Blake and family even cooked us meals and sent gift cards. The phrase it takes a village really came to life during this time.
Advice for NICU Parents:
1. Develop a schedule/ plan for yourself.
2. Take time for yourself when you are not visiting (take an extra long shower, go get your favorite meal, etc)
3. Stay on top of vitamins/ nutrition. The NICU is draining and emotionally/ physically exhausting. You need to be in your best health
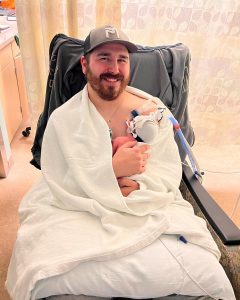
4. Hold/ touch/ talk to your baby. They know your voice. You are their safe place.
In an environment where they are poked/ man handled (not intentionally), you need to be calm.
Present day:
Blake is now 7 weeks old and is picking up his head more during tummy time/ is awake for longer periods. He also is louder in his screams/ cries (he used to sound like a little bird).
louder in his screams/ cries (he used to sound like a little bird).
